Hammer Toes Symptoms
Hammertoes usually start out as mild deformities and get progressively worse over time. In the earlier stages, hammertoes are flexible and the symptoms can often be managed with changes in shoe styles and foot care products. But if left untreated, hammertoes can become more rigid and painful. Corns are more likely to develop as time goes on-and corns never really go away, even after trimming. In more severe cases of Hammer toes, corn lesions may evolve into severe ulcerations. These lesions frequently occur in patients who have vascular disease or are Diabetic with neuropathy. The ulcerations can extend to the bone and result in infection and possible loss of digit or amputation.
Causes
As described above, the main reason people develop hammertoes is improper footwear, or footwear that is too short for the toes. Shoes that do not allow our toes to lie flat are the biggest cause of hammertoes, though there are others, including genetics, injury or trauma in which the toe is jammed or broken. Diseases that affect the nerves and muscles, such as arthritis. Abnormal foot mechanics due to nerve or muscle damage, causing an imbalance of the flexor and extensor tendons of the toe. Systematic diseases such as arthritis can also lead to problems such as hammertoe. Some people are born with hammertoes, while others are more prone to developing the condition due to genetics. If you have ever broken a toe, you know there is not much that can be done for it. It is one of the only bones in the body that heals without the use of a cast. A broken toe may be splinted, however, which may help prevent a hammertoe from forming.
 Symptoms
Symptoms
If you have any of these symptoms, do not assume it is due to hammer toe. Talk to your doctor about symptoms such as a toe that curls down, corns on the top of a toe, calluses on the sole of the foot or bottom of the toe, pain in the middle joint of a toe, discomfort on the top of a toe, difficulty finding any shoes that fit comfortably, cramping in a toe, and sometimes also the foot and leg, difficult or painful motion of a toe joint, pain in the ball of the foot or at the base of a toe.
Diagnosis
Some questions your doctor may ask of you include, when did you first begin having foot problems? How much pain are your feet or toes causing you? Where is the pain located? What, if anything, seems to improve your symptoms? What, if anything, appears to worsen your symptoms? What kind of shoes do you normally wear? Your doctor can diagnose hammertoe or mallet toe by examining your foot. Your doctor may also order X-rays to further evaluate the bones and joints of your feet and toes.
Non Surgical Treatment
Non-surgical methods for hammer toes (claw toes) are aimed at decreasing symptoms (i.e., pain and/or calluses) and/or limiting the progression into a larger problem. Simple treatments patients can do are wear supportive shoes. Use an arch support. Wear shoes hammertoes with a wide toe box. Modify activities. Spot stretch shoes. Periodic callus care.
Surgical Treatment
Sometimes when the joints are removed the two bones become one as they are fused in a straightened position. Many times one toe will be longer than another and a piece of bone is removed to bring the toes in a more normal length in relation to each other. Sometimes tendons will be lengthened, or soft tissue around the joints will be cut or rebalanced to fix the deformity. Angular corrections may also be needed. The surgeon may place fixation in your foot as it heals which may include a pin, or wires.
 Prevention
Prevention
Custom orthotics paired with a well made shoe can prevent the progression and development of hammertoes. Wearing proper-fitting shoes and custom orthotic devices can provide the support patients need to address muscle/tendon dysfunction. It can also support end stage diseases that result in hammertoe deformities by re-balancing the foot and ankle and controlling the deforming forces.
Help For Hammer Toe Pain
 Overview
Overview
A hammertoes is a term that is commonly used to describe any type of toe deformity. It is a common problem that may or may not be a problem. What does a hammer toe look like? In a hammertoe the deformity usually exists in one toe (at the proximal inter phalangeal joint) - the base of the toe points upward and the end of the toe points down.
Causes
Hammer toes result from a muscle imbalance which causes the ligaments and tendons to become unnaturally tight. This results in the joint curling downward. Arthritis can also lead to many different forefoot deformities, including hammer toes.
 Symptoms
Symptoms
The most common symptoms of hammertoes include. The toe is bent upward at the middle toe joint, so that the top of this joint rubs against the top of the shoe. The remainder of the toe is bent downward. Pain upon pressure at the top of the bent toe from footwear. The formation of corns on the top of the joint. Redness and swelling at the joint contracture. Restricted or painful motion of the toe joint. Pain in the ball of the foot at the base of the affected toe. This occurs because the contracted digit puts pressure on the metatarsal head creating callouse and pressure on the ball of the foot.
Diagnosis
A hammertoe is usually diagnosed with a physical inspection of your toe. Imaging tests, such as X-rays, may be ordered if you have had a bone, muscle, or ligament injury in your toe.
Non Surgical Treatment
Your podiatrist may recommend conservative treatment techniques for your hammertoes based on your foot structure, which will likely involve removing any thick, painful skin, padding your painful area, and recommending for you shoes that give your curled toes adequate hammertoes room. Conservative care strategies for this health purpose may also involve the use of Correct Toes, our toe straightening and toe spacing device.
Surgical Treatment
In advanced cases in which the toe has become stiff and permanently bent, the toe can be straightened with surgery. One type of surgery involves removing a small section of the toe bone to allow the toe to lie flat. Surgery for hammertoe usually is classified as a cosmetic procedure. Cosmetic foot surgeries sometimes cause complications such as pain or numbness, so it?s better to treat the problem with a shoe that fits properly.
Over-Pronation
Overview
If the inner side of your shoes are especially worn, you could be overpronating. Excessive inward roll of the foot after landing, such that the foot continues to roll when it should be pushing off. This twists the foot, shin and knee and can cause pain in all those areas. If you are an overpronator, you'll find excessive wear on the inner side of your shoes, and they'll tilt inward if you place them on a flat surface. Knock knees or flat feet contribute to overpronation.

Causes
In adults, the most common reason for the onset of Over-Pronation is a condition known as Post Tibial Tendonitis. This condition develops from repetitive stress on the main supporting tendon (Posterior Tibial Tendon) of the foot arch. As the body ages, ligaments and muscles can weaken. When this occurs the job of providing the majority of the support required by the foot arch is placed upon this tendon. Unfortunately, this tendon cannot bear the weight of this burden for too long. Eventually it fatigues under the added strain and in doing so the foot arch becomes progressively lower over a period of time.
Symptoms
Due to the laxity of the soft tissue structures of the foot, and the fact that the joints are not held together properly, the bones of the feet shift. When this occurs, the muscles that attach to these bones must also shift, or twist, in order to attach to these bones. The strongest and most important muscles that attach to our foot bones come from our lower leg. So, as these muscles course down the leg and across the ankle, they must twist to maintain their proper attachments in the foot. This twisting of these muscles will cause shin splints, Achilles Tendonitis, generalized tendonitis, fatigue, muscle aches and pains, cramps, ankle sprains, and loss of muscular efficiency (reducing walking and running speed and endurance). The problems we see in the feet, which are due to over-pronation include bunions, heel spurs, plantar fasciitis, fallen and painful arches, hammertoes, metatarsalgia (ball of foot pain), and calluses.
Diagnosis
Look at your soles of your footwear: Your sneaker/shoes will display heavy wear marks on the outside portion of the heel and the inside portion above the arch up to the top of the big toe on the sole. The "wet-foot" test is another assessment. Dip the bottom of your foot in water and step on to a piece of paper (brown paper bag works well). Look at the shape of your foot. If you have a lot of trouble creating an arch, you likely overpronate. An evaluation from a professional could verify your foot type.

Non Surgical Treatment
Treatment with orthotics will provide the required arch support to effectively reduce excessive pronation and restore the foot and its posture to the right biomechanical position. It should be ensured that footwear has sufficient support, for example, shoes should have a firm heel counter to provide adequate control.
Surgical Treatment
Depending on the severity of your condition, your surgeon may recommend one or more treatment options. Ultimately, however, it's YOUR decision as to which makes the most sense to you. There are many resources available online and elsewhere for you to research the various options and make an informed decision.
What Are The Chief Causes Of Severs Disease?
Overview
Sever?s Disease is used to describe pain in the back of the heel that comes from an inflamed growth plate in your child?s heel. Sever?s Disease commonly occurs in children from the ages 8-15. The muscles and tendons become tight as the bones shift and grow. This causes pain when walking or participating in athletic events that require running and jumping.
Causes
Sever?s disease is most likely to occur during the growth spurt that occurs in adolescence. For girls, growth spurts usually occurs between 8 and 13 years of age. For boys, it?s typically between 10 and 15 years of age. The back of the heel hardens and becomes stronger when it finishes growing, which is why Sever?s rarely occurs in older adolescents and teenagers.
Symptoms
As a parent, you may notice your child limping while walking or running awkwardly. If you ask them to rise onto their tip toes, their heel pain usually increases. Heel pain can be felt in one or both heels in Sever's disease.
Diagnosis
To diagnose the cause of the child?s heel pain and rule out other more serious conditions, the foot and ankle surgeon obtains a thorough medical history and asks questions about recent activities. The surgeon will also examine the child?s foot and leg. X-rays are often used to evaluate the condition. Other advanced imaging studies and laboratory tests may also be ordered.
Non Surgical Treatment
Reduce inflammation:
Ice: For at least 20 minutes after activity or when pain increases.
Nonsteroidal anti-inflammatory drugs:(NSAIDs) may also help. Stretch the calf. Increase calf flexibility by doing calf stretches for 30 to 45 seconds several times per day.
Protect the heel: The shoe may need to be modified to provide the proper heel lift or arch support.
Select a shoe with good arch support and heel lift if possible. Try heel lifts or heel cups in sports shoes, especially cleats. Try arch support in cleats if flat feet contribute to the problem.
Take it one step at a time:. Gradually resume running and impact activities as symptoms allow. Sever?s disease usually goes away when the growth plate (apophysis) matures, which should be by age 12 to 13 years in females and 13 to 14 years in males.
Understanding Heel Soreness
Overview
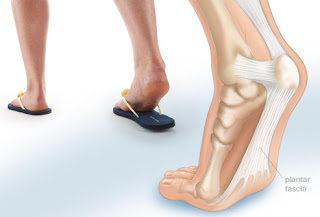
Heel pain can be very aggravating, especially when taking those first steps in the morning. The key to decreasing and possibly eliminating Heel Pain is to stretch your heel cord and plantar fascia. The heel cord is the Achilles tendon, which connects the gastrocnemius and soleus muscles in the calf to the heel bone. The plantar fascia is a thick tissue that runs along the bottom of your foot, connecting the heel bone to the toes and maintaining the arch.
Causes
Plantar fasciitis is caused by inflammation and irritation of the tight tissue forming the arch of the foot. The most common cause of heel pain, it typically affects men, aged 40 - 70 who are physically active. The bottom or inside of the foot and / or heel (where heel and arch meet) may hurt or cause severe pain upon standing after resting -- or most often, when arising in the morning. The pain is usually experienced within the first few steps and is often characterized as "walking on nails" or knife blades. The pain may let up after walking a bit but most commonly returns after prolonged movement or a rest.
Symptoms
The symptoms of plantar fasciitis are classically pain of a sharp nature which is worse standing first thing in the morning. After a short period of walking the pain usually reduces or disappears, only to return again later in the day. Aggravating times are often after increased activity and rising from sitting. If these are the sort of symptoms you are experiencing then the Heel-Fix Kit ? will be just the treatment your heel is crying out for. Some heel pain is more noticeable at night and at rest. Because plantar fasciitis is a mechanical pathology it is unlikely that this sort of heel pain is caused by plantar fasciitis. The most common reason for night heel pain is pressure on your Sciatic nerve causing referred pain in the heel. Back pain is often present as well, but you can get the heel pain with little or no back pain that is caused by nerve irritation in the leg or back. If you get pain in your heels mainly or worse at night please see a clinician as soon as you can to confirm the diagnosis.
Diagnosis
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
Non Surgical Treatment
If you have experienced painful heels try wearing your shoes around your house in the evening. Don't wear slippers or socks or go barefoot. You may also try gentle calf stretches for 20 to 30 seconds on each leg. This is best done barefoot, leaning forward towards a wall with one foot forward and one foot back. If the pain persists longer than one month, you should visit a podiatrist for evaluation and treatment. Your feet should not hurt, and professional podiatric care may be required to help relieve your discomfort. If you have not exercised in a long time, consult your podiatric physician before starting a new exercise program. Begin an exercise program slowly. Don't go too far or too fast. Purchase and maintain good shoes and replace them regularly. Stretch each foot and achilles tendon before and after exercise. Avoid uneven walking surfaces or stepping on rocks as much as possible. Avoid going barefoot on hard surfaces. Vary the incline on a treadmill during exercise. Nobody walks uphill all the time. If it hurts, stop. Don't try to "work through the pain." Your podiatric physician/surgeon has been trained specifically and extensively in the diagnosis and treatment of all manner of foot conditions. This training encompasses all of the intricately related systems and structures of the foot and lower leg including neurological, circulatory, skin, and the musculoskeletal system, which includes bones, joints, ligaments, tendons, muscles, and nerves.
Surgical Treatment
Extracorporeal shockwave therapy (EST) is a fairly new type of non-invasive treatment. Non-invasive means it does not involve making cuts into your body. EST involves using a device to deliver high-energy soundwaves into your heel. The soundwaves can sometimes cause pain, so a local anaesthetic may be used to numb your heel. It is claimed that EST works in two ways. It is thought to have a "numbing" effect on the nerves that transmit pain signals to your brain, help stimulate and speed up the healing process. However, these claims have not yet been definitively proven. The National Institute for Health and Care Excellence (NICE) has issued guidance about the use of EST for treating plantar fasciitis. NICE states there are no concerns over the safety of EST, but there are uncertainties about how effective the procedure is for treating heel pain. Some studies have reported that EST is more effective than surgery and other non-surgical treatments, while other studies found the procedure to be no better than a placebo (sham treatment).
Prevention

A variety of steps can be taken to avoid heel pain and accompanying afflictions. Wear shoes that fit well-front, back, and sides-and have shock-absorbent soles, rigid shanks, and supportive heel counters. Wear the proper shoes for each activity. Do not wear shoes with excessive wear on heels or soles. Prepare properly before exercising. Warm up and do stretching exercises before and after running. Pace yourself when you participate in athletic activities. Don?t underestimate your body's need for rest and good nutrition. If obese, lose weight.
What Should I Do About Achilles Tendinitis ?
Overview
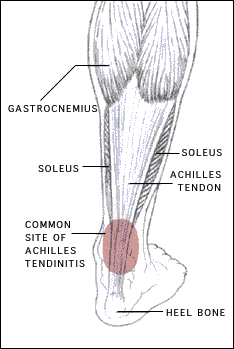
 Achilles tendonitis is a condition wherein the Achilles tendon, at or near its insertion to back of the heel, becomes inflamed and causes pain. The Achilles tendon is one of the longest and strongest tendons in the body. It is avascular (not supplied with blood vessels) so it can be slow to heal. The Achilles tendon is formed in the lower third of the leg. Two muscles join to form the Achilles tendon, the Gastrocnemius and the Soleus which are commonly referred to as the calf muscle. The Achilles tendon works as an anti-pronator which means it helps to prevent the foot from rolling inward.
Achilles tendonitis is a condition wherein the Achilles tendon, at or near its insertion to back of the heel, becomes inflamed and causes pain. The Achilles tendon is one of the longest and strongest tendons in the body. It is avascular (not supplied with blood vessels) so it can be slow to heal. The Achilles tendon is formed in the lower third of the leg. Two muscles join to form the Achilles tendon, the Gastrocnemius and the Soleus which are commonly referred to as the calf muscle. The Achilles tendon works as an anti-pronator which means it helps to prevent the foot from rolling inward.
Causes
The majority of Achilles tendon injuries are due to overuse injuries. Other factors that lead to Achilles tendonitis are improper shoe selection, inadequate stretching prior to engaging in athletics, a short Achilles tendon, direct trauma (injury) to the tendon, training errors and heel bone deformity. There is significant evidence that people with feet that role in excessively (over-pronate) are at greater risk for developing Achilles tendinitis. The increased pronation puts additional stress on the tendon, therefore, placing it at greater risk for injury.
Symptoms
The onset of the symptoms of Achilles tendonitis tend to be gradual, with symptoms usually developing over a period of several days, or even weeks. Symptoms may include, Pain, this may be mild at first and may only be noticeable after exercise. Over time the pain may become constant and severe. Stiffness, this is usually relieved by activity. Sluggishness in the leg. Tenderness, particularly in the morning and most commonly felt just above where the tendon attaches to the heel bone. Swelling.
Diagnosis
If you think you have Achilles tendinitis, make an appointment to see your doctor. The doctor will ask you questions about your recent activity and look for signs. The foot not flexing when the calf muscle is pressed ( if Achilles ruptures or tears in half). Swelling on the back of the foot. Pain in the back of the foot. Limited range of motion in ankle. An X-ray or MRI scan can check for tendinitis.
Nonsurgical Treatment
Take a course (5 - 7 days) of non-steroidal anti-inflammatory drugs(ibuprofen/voltaren/cataflam/mobic) available from your general practitioner or pharmacist. Apply ice to the Achilles - for 10 minutes every 2 hours, in order to reduce the inflammation. Avoid weight-bearing activities and keep foot elevated where possible. Self-massage - using arnica oil or anti-inflammatory gel. Rub in semi-circles in all directions away from the knotted tissue, three times a day once the nodule is gone, stretch the calf muscle gently do not start running until you can do heel raises and jumping exercises without pain return to running gradually full recovery is usually between six to eight weeks.

Surgical Treatment
There are two types of Achilles repair surgery for tendonitis (inflammation of the Achilles Tendon), if nonsurgical treatments aren't effective. Gastrocnemius recession - The orthopaedic surgeon lengthens the calf muscles to reduce stress on your Achilles tendon. D?bridement and repair - During this procedure, the surgeon removes the damaged part of the Achilles tendon and repairs the remaining tendon with sutures or stitches. Debridement is done when the tendon has less than 50% damage.
Prevention
Although Achilles tendinitis cannot be completely prevented, the risk of developing it can be lowered. Being aware of the possible causes does help, but the risk can be greatly reduced by taking the following precautions. Getting a variety of exercise - alternating between high-impact exercises (e.g. running) and low-impact exercise (e.g. swimming) can help, as it means there are days when the Achilles tendon is under less tension. Limit certain exercises - doing too much hill running, for example, can put excessive strain on the Achilles tendon. Wearing the correct shoes and replacing them when worn - making sure they support the arch and protect the heel will create less tension in the tendon. Using arch supports inside the shoe, if the shoe is in good condition but doesn't provide the required arch support this is a cheaper (and possibly more effective) alternative to replacing the shoe completely. Stretching, doing this before and after exercising helps to keep the Achilles tendon flexible, which means less chance of tendinitis developing. There is no harm in stretching every day (even on days of rest), as this will only further improve flexibility. Gradually increasing the intensity of a workout - Achilles tendinitis can occur when the tendon is suddenly put under too much strain, warming up and increasing the level of activity gradually gives your muscles time to loosen up and puts less pressure on the tendon.
What Leads To Heel Discomfort

Overview
Heel pain is most commonly caused by plantar fasciitis, which is the swelling of the tissue that connects the heel bone to the toes at the bottom part of the foot, also known as the plantar fascia. Plantar fasciitis is often described as sharp pain in the middle of the heel, which is typically worse after periods of rest when fascia contracts. The pain usually becomes more bearable as the muscles loosen up during the low-impact walking, but can return even worse after extended periods of walking or standing. The plantar fascia serves as a shock absorber and supports the foot’s arch. Too much tension on the plantar fascia can cause inflammation and swelling. Fortunately in most cases, plantar fasciitis treatment is fairly conservative. Plantar fasciitis exercises, medications and orthotics are usually all that’s needed to manage the pain. Most severe cases may require surgery.
Causes
Patients with tight calf muscles will suffer with excessive pulling of the muscle group on the back of the heel. This in turn creates pulling of other structures that are attached to the heel, including the Plantar Fascia. When the pulling continues for long enough, then inflammation will develop and lead to Plantar Fasciitis. This causes Heel Pain. It is extremely common for patients who increase their level of activity to develop Plantar Fasciitis. Boot camp, running, zumba, recreational walking or other quick movement sports such as tennis or touch football are typical causes of Heel Pain. The sharp increase in exercise is too much for the foot to cope with and the stress on the Plantar Fascia causes inflammation. The Heel Pain that is caused by this inflammation is known as Plantar Fasciitis.
Symptoms
Symptoms of plantar fasciitis can occur suddenly or gradually. When they occur suddenly, there is usually intense heel pain on taking the first morning steps, known as first-step pain. This heel pain will often subside as you begin to walk around, but it may return in the late afternoon or evening. When symptoms occur gradually, a more long-lasting form of heel pain will cause you to shorten your stride while running or walking. You also may shift your weight toward the front of the foot, away from the heel.
Diagnosis
After you describe your symptoms and discuss your concerns, your doctor will examine your foot. Your doctor will look for these signs. A high arch, an area of maximum tenderness on the bottom of your foot, just in front of your heel bone. Pain that gets worse when you flex your foot and the doctor pushes on the plantar fascia. The pain improves when you point your toes down. Limited "up" motion of your ankle. Your doctor may order imaging tests to help make sure your heel pain is caused by plantar fasciitis and not another problem. X-rays provide clear images of bones. They are useful in ruling out other causes of heel pain, such as fractures or arthritis. Heel spurs can be seen on an x-ray. Other imaging tests, such as magnetic resonance imaging (MRI) and ultrasound, are not routinely used to diagnose plantar fasciitis. They are rarely ordered. An MRI scan may be used if the heel pain is not relieved by initial treatment methods.
Non Surgical Treatment
Many cases of plantar fasciitis can be treated with simple, conservative measures. These include ice packs, stretching exercises, anti-inflammatory medications, orthotic devices (custom molded orthotics), and physical therapy. It’s important to consult your doctor before you take any medications to treat this condition. In chronic or persistent cases, one of three techniques may be used to treat plantar fasciitis. Extracorporeal Shock Wave Treatment (ESWT). TOPAZ treatment. Platelet Rich P
lasma therapy.

Surgical Treatment
In unusual cases, surgical intervention is necessary for relief of pain. These should only be employed after non-surgical efforts have been used without relief. Generally, such surgical procedures may be completed on an outpatient basis in less than one hour, using local anesthesia or minimal sedation administrated by a trained anesthesiologist. In such cases, the surgeon may remove or release the injured and inflamed fascia, after a small incision is made in the heel. A surgical procedure may also be undertaken to remove bone spurs, sometimes as part of the same surgery addressing the damaged tissue. A cast may be used to immobilize the foot following surgery and crutches provided in order to allow greater mobility while keeping weight off the recovering foot during healing. After removal of the cast, several weeks of physical therapy can be used to speed recovery, reduce swelling and restore flexibility.
Stretching Exercises
Stretching exercises for your foot are important. Do the stretches shown here at least twice a day. Don't bounce when you stretch. Plantar fascia stretch. To do the plantar fascia stretch, stand straight with your hands against a wall and your injured leg slightly behind your other leg. Keeping your heels flat on the floor, slowly bend both knees. You should feel the stretch in the lower part of your leg. Hold the stretch for 10 to 15 seconds. Repeat the stretch 6 to 8 times. Calf stretch. Stand with your hands against a wall and your injured leg behind your other leg. With your injured leg straight, your heel flat on the floor and your foot pointed straight ahead, lean slowly forward, bending the other leg. You should feel the stretch in the middle of your calf. Hold the stretch for 10 to 15 seconds. Repeat the stretch 6 to 8 times. Other exercises. You can also strengthen your leg muscles by standing on the ball of your foot at the edge of a step and raising up as high as possible on your toes. Relax between toe raises and let your heel fall a little lower than the edge of the step. It's also helpful to strengthen the foot by grabbing a towel with your toes as if you are going to pick up the towel with your foot. Repeat this exercise several times a day.
Symptoms Of Nail Conditions
Pain across the bottom of the foot at any point between the heel and the ball of the foot is often referred to as "arch pain” Although this description is non-specific, most arch pain is due to strain or inflammation Bunions Callous of the plantar fascia (a long ligament on the bottom of the foot). Wearing inappropriate footwear or foot problems like athlete's foot and Morton's neuroma are some of the factors that cause burning feet sensation.
TOE CONDITIONS: Ingrown toenails, blood accumulation under the nail plate (subungual hematoma), corns and calluses are all often seen as a result of playing baseball. It is important that good foot hygiene be practiced with washing between the toes and drying the feet well after bathing. Topical antifungals work well to treat athletes foot. ORTHOPEDIC INJURIES: Most orthopedic baseball foot and ankle injuries are acute or sudden. If an individuals foot or ankle is injured, seek immediate evaluation with one of our doctors. If your athlete has a baseball related injury, call our specialists at Advanced Foot and Ankle Center in McKinney and Prosper Texas at 972-542-2155. However, toe numbness and pain occurring together is one such problem that you cannot afford to ignore. Common symptoms are flat feet knee problems , burning sensation, numbness.
When the tissue of the arch of the foot becomes irritated and inflamed, even simple movements can be quite painful. Plantar fasciitis is the name that describes inflammation of the fibrous band of tissue that connects the heel to the toes. Symptoms of plantar fasciitis include pain early in the morning and pain with long walks or prolonged standing. Arch pain early in the morning is due to the plantar fascia becoming contracted and tight as you sleep through the night. Bunions develop from a weakness in the bone structure of your foot.

On the other hand, the surgical hip pain treatment includes total hip bone replacement surgery. Although it is always advisable to consult the doctor if you experience pain in the hip that lasts for more than a couple of hours, you can try some home remedies to temporarily get rid of the sharp hip pain. One should note that these home remedies are not to be substituted for proper medical treatment. Ice packs and cool compresses are helpful to ease pain and inflammation on various parts of the body. Rest and ice the sole of your feet.

During the average lifetime our feet cover over 70,000 miles, the equivalent of walking four times around the world., so it's not surprising that problems can occur. Indeed around three-quarters of all adults will experience some sort of problem with their feet at some time. And without treatment most foot complaints will become gradually worse with time. This means people often endure painful conditions for far too long, and the problem can get worse. People often assume nothing can be done to help their condition, but in fact these conditions are extremely treatable. Swollen lump on big toe joint; lump may become numb but also make walking painful.
All About Achilles Tendonitis
Overview
 Achilles tendinitis is an inflammation of your Achilles tendon. It?s quite common in people who have psoriatic arthritis, reactive arthritis or ankylosing spondylitis. It can also occur as an over-use injury in people who take part in excessive exercise or exercise that they?re not used to.
Achilles tendinitis is an inflammation of your Achilles tendon. It?s quite common in people who have psoriatic arthritis, reactive arthritis or ankylosing spondylitis. It can also occur as an over-use injury in people who take part in excessive exercise or exercise that they?re not used to.
Causes
Achilles tendonitis is a common sports injury caused by repeated or intense strain on the tendon. But non-athletes also can get it if they put a lot of stress on their feet. Other things that contribute to Achilles tendonitis include. An increase in activity. Starting a training program after a period of inactivity or adding miles or hills to a jogging regimen are two examples of things that put people at risk for Achilles tendonitis. Sports that require sudden starts and stops; for example, tennis and basketball. A change in footwear, or wearing old or badly fitting shoes. New shoes, worn-out shoes, or the wrong size shoes can cause a person's feet to overcompensate and put stress on the Achilles tendon. Additionally, wearing high heels all the time can cause the tendon and calf muscles to get shorter, and the switch to flat shoes and exercise can put extra strain on the heel. Running up hills. Going uphill forces the Achilles tendon to stretch beyond its normal range. Weak calf muscles, flat arches, "overpronation" (feet that roll in when running), or "oversupination" (feet that roll out when running). Overpronation and oversupination make the lower leg rotate and put a twisting stress on the tendon. Exercising without warming up. Tight calf muscles or muscles that lack flexibility decrease a person's range of motion and put an extra strain on the tendon. Running or exercising on a hard or uneven surface or doing lunges or plyometrics without adequate training. A traumatic injury to the Achilles tendon.
Symptoms
Symptoms of Achilles tendinitis and tendinosis include recurring localized heel pain, sometimes severe, along the achilles tendon during or after exercise. Pain often begins after exercise and gradually worsens. Morning tenderness or stiffness about an inch and a half above the point where the Achilles tendon is attached to the heel bone. Sluggishness in your leg. Mild to severe swelling. Stiffness that generally diminishes as the tendon warms up with use.
Diagnosis
A podiatrist can usually make the diagnosis by clinical history and physical examination alone. Pain with touching or stretching the tendon is typical. There may also be a visible swelling to the tendon. The patient frequently has difficulty plantarflexing (pushing down the ball of the foot and toes, like one would press on a gas pedal), particularly against resistance. In most cases X-rays don't show much, as they tend to show bone more than soft tissues. But X-rays may show associated degeneration of the heel bone that is common with Achilles Tendon problems. For example, heel spurs, calcification within the tendon, avulsion fractures, periostitis (a bruising of the outer covering of the bone) may all be seen on X-ray. In cases where we are uncertain as to the extent of the damage to the tendon, though, an MRI scan may be necessary, which images the soft tissues better than X-rays. When the tendon is simply inflamed and not severely damaged, the problem may or may not be visible on MRI. It depends upon the severity of the condition.
Nonsurgical Treatment
The initial aim of the treatment in acute cases is to reduce strain on the tendon and reduce inflammation until rehabilitation can begin. This may involve, avoiding or severely limiting activities that may aggravate the condition, such as running or uphill climbs. Using shoe inserts (orthoses) to take pressure off the tendon. Wear supportive shoes. Reducing Inflammation by icing. Taking non-steroidal anti-inflammatory drugs. Heel cups and heel lifts can be used temporarily to take pressure off the tendon, but must not be used long term as it can lead to a shortening of the calf. Calf Compression Sleeves. Placing the foot in a cast or restrictive ankle-boot to minimize movement and give the tendon time to heal. This may be recommended in severe cases and used for about eight weeks.
Surgical Treatment
Achilles tendon repair surgery is often used to repair a ruptured or torn Achilles tendon, the strong fibrous cord that connects the two large muscles in the back of your calf to your heel bone. These muscles (the gastrocnemius and the soleus) create the power needed to push off with your foot or rise up on your toes. Achilles tendon ruptures are quite common. Most happen during recreational activities that require sudden bursts of muscle power in the legs. Often a torn Achilles tendon can be diagnosed with a physical examination. If swelling is present, the orthopaedist may delay the Achilles tendon surgery until it subsides.
Prevention
Suggestions to reduce your risk of Achilles tendonitis include, incorporate stretching into your warm-up and cool-down routines, maintain an adequate level of fitness for your sport, avoid dramatic increases in sports training, if you experience pain in your Achilles tendon, rest the area. Trying to ?work through? the pain will only make your injury worse, wear good quality supportive shoes appropriate to your sport. If there is foot deformity or flattening, obtain orthoses, avoid wearing high heels on a regular basis. Maintaining your foot in a ?tiptoe? position shortens your calf muscles and reduces the flexibility of your Achilles tendon. An inflexible Achilles tendon is more susceptible to injury, maintain a normal healthy weight.
Concerning Achilles Tendinitis
Overview
 Achilles tendinitis is very common among running athletes. The calf muscles attach to the calcaneus via the Achilles tendon. During running, the calf muscles help with the lift-off phase of gait. Repetitive forces from running combined with insufficient recovery time can initially cause inflammation in the tendon paratenon (fatty areolar tissue that surrounds the tendon). A complete tear of the Achilles tendon is a serious injury, usually resulting from sudden, forceful stress. Tendon tears can occur with minimal exertion in people who have taken fluoroquinolone antibiotics.
Achilles tendinitis is very common among running athletes. The calf muscles attach to the calcaneus via the Achilles tendon. During running, the calf muscles help with the lift-off phase of gait. Repetitive forces from running combined with insufficient recovery time can initially cause inflammation in the tendon paratenon (fatty areolar tissue that surrounds the tendon). A complete tear of the Achilles tendon is a serious injury, usually resulting from sudden, forceful stress. Tendon tears can occur with minimal exertion in people who have taken fluoroquinolone antibiotics.
Causes
Achilles tendinitis usually results from overuse and not a specific injury or trauma. When the body is subject to repetitive stress, the Achilles tendon is more prone to become inflamed. Other factors may cause Achilles tendinitis, such as, Sudden increase in physical activity, which can be related to distance, speed or hills, without giving yourself adequate time to adjust to the heightened activity. With running up hills, the Achilles tendon has to stretch more for each stride, which creates rapid fatigue. Inadequate footwear or training surface. High heels may cause a problem, because the Achilles tendon and calf muscles are shortened. While exercising in flat, athletic shoes, the tendon is then stretched beyond its normal range, putting abnormal strain on the tendon. Tight calf muscles which gives the foot a decreased range of motion. The strained calf muscles may also put extra strain on the Achilles tendon. Bone spur where the Achilles tendon attaches to the heel bone, aggravating the tendon and causing pain.
Symptoms
There will be a gradual onset of achilles tendon pain over a period of weeks, or even months. The pain will come on during exercise and is constant throughout the training session. Pain will be felt in the achilles tendon when walking especially up hill or up stairs. This is because the achilles is having to stretch further than normal. There is likely to be stiffness in the Achilles tendon especially in the morning or after a long period of rest. This is thought to be due to adhesions between the tendon sheath and the tendon itself. Nodules or lumps may be found in the achilles tendon, particularly 2-4cm above the heel and the skin will appear red. Pain and tenderness will be felt when pressing in on the achilles tendon which is likely to appear thickened or swollen. A creaking sensation may be felt when press the fingers into the sides of the tendon and moving the ankle.This is known as crepitus.
Diagnosis
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose an Achilles injury such as Achilles tendonitis. Occasionally, further investigations such as an Ultrasound, X-ray or MRI scan may be required to assist with diagnosis and assess the severity of the condition.
Nonsurgical Treatment
Achilles tendinitis can typically be treated at home by following the R.I.C.E. treatment method. Rest. Rest the tendon by avoiding activities that irritate the tendon or increase swelling. However, this does not mean you should be completely inactive for long periods of time, as this can cause stiffness in your joints. It?s still important to stretch in order to maintain strength and flexibility and partake in activities that don?t put direct pressure on the tendon, such as bicycling. Ice. Apply ice to the affected area for 20-minutes at a time, every couple hours, as needed, to reduce swelling and pain. Compression. Use compression bandages to help reduce swelling. Elevation. Elevate your ankle above the level of your heart to help reduce swelling. It is particularly important to do this at night while you sleep. Simply place a pillow or two under your ankle to keep it elevated. Once the tendon has healed, be sure to gradually return to more strenuous activities. If flattened arches contributed to the injury, wear shoes with appropriate support or inserts to prevent the condition from progressing or recurring. If these non-surgical treatments have not been able to provide relief of symptoms after several months, surgery may be performed to remove inflamed tissue. However, this is not usually recommended unless all other options have been exhausted. Consult your doctor for more information about surgical treatment options.

Surgical Treatment
Your doctor may recommend surgery if, after around six months, other treatments haven?t worked and your symptoms are having an impact on your day-to-day life. Surgery involves removing damaged areas of your tendon and repairing them.
Prevention
While it may not be possible to prevent Achilles tendinitis, you can take measures to reduce your risk. Increase your activity level gradually. If you're just beginning an exercise regimen, start slowly and gradually increase the duration and intensity of the training. Take it easy. Avoid activities that place excessive stress on your tendons, such as hill running. If you participate in a strenuous activity, warm up first by exercising at a slower pace. If you notice pain during a particular exercise, stop and rest. Choose your shoes carefully. The shoes you wear while exercising should provide adequate cushioning for your heel and should have a firm arch support to help reduce the tension in the Achilles tendon. Replace your worn-out shoes. If your shoes are in good condition but don't support your feet, try arch supports in both shoes. Stretch daily. Take the time to stretch your calf muscles and Achilles tendon in the morning, before exercise and after exercise to maintain flexibility. This is especially important to avoid a recurrence of Achilles tendinitis. Strengthen your calf muscles. Strong calf muscles enable the calf and Achilles tendon to better handle the stresses they encounter with activity and exercise. Cross-train. Alternate high-impact activities, such as running and jumping, with low-impact activities, such as cycling and swimming.
Print "Symptoms Associated With Side Of Foot Pain"
Plantar fasciitis usually involves pain and inflammation at the bottom of your foot that connects your heel bone to your toes. A survey done by the American Podiatric Medical Association revealed that 64 % of people suffering from heel pain have never sought treatment from a podiatric physician.
Corns can form under a callus on the ball of the foot which will be very painful. You must concern with doctor regarding the pain or the issue behind this foot pain. One of the common factors behind foot pain is your designer shoes. If any kind of doubt strikes in your mind, concern with an expert foot surgeon or health professionals. Ignorance of any foot pain only causes trouble to your own health and fitness. Denial Bob is associated with , and writes more about foot pain and the treatment mentioned by foot surgeon. The pain from stress fractures usually decreases with rest and increases with activity. Apply ice to the foot and take an over-the-counter anti-inflammatory medicine to relieve pain. Your pain may be from DAMAGE TO THE SKIN OR TENDONS on top of the foot. See your doctor if the pain doesn't get better within a few days. Apply ice to reduce the swelling and take an over-the-counter analgesic such as ibuprofen to help relieve pain. See your doctor if your pain doesn't get better.
Neuromas & recommended shoes - Caused by a benign nerve growth, pain is usually felt between the third and fourth toes. Posterior Tibia Tendonitis & recommended shoes - Pain in the inside of the foot and ankle, and on occasion problems associated with an unstable gait. Metatarsalgia & recommended shoes - A condition marked by pain and inflammation in the ball of your foot. Because the feet are very small compared with the rest of the body, the impact of each step exerts tremendous force upon them. During a typical day, people spend about 4 hours on their feet and take 8,000 - 10,000 steps. This means that the feet support a combined force equivalent to several hundred tons every day. The hindfoot is the back of the foot.
Sprain: When the fibers of the tissue tear due to overstretched ligaments, a sprain occurs, and a sprain is known to cause extreme pain. Muscle Injury: Overloading, overuse, over-stretching, or bruising of the muscles and tendons of the foot may lead to severe pain in the foot. Plantar Fasciitis: Planter fascia strains are generally felt as the pain at the bottom of the foot. This condition is known as plantar fasciitis. Wrong Shoes: Wearing narrow toed shoes may lead to development of a bunion, a big, hard, and painful protrusion at the base of the big toe, causing pain in the foot. Hammer Toes: As contraction of muscles leads to hammer or curled toes, it is often a cause of severe pain.
I recently stopped wearing them for a few months, and the heel pain returned, so I'm ordering more for my shoes. When I initially put your inserts into my shoes, they felt a bit strange, especially in my arches. Shoes with high heels can create much trouble for your feet.

Movement of the foot is controlled by four groups of muscles in the leg. These muscles get a workout not only when our feet are visibly moving (such as when we walk or run) but even when we stand still, because they help keep us balanced and upright. And like nearly all muscles (the heart muscle is an exception), these muscles can become fatigued, decreasing their ability to properly support the feet and causing discomfort. Here are some common problems that cause foot pain, most often due to an overuse injury. Bad shoes cause foot and ankle problems.

Light and washable, they also have specially designed air vents to help keep your feet cool. We'll also include this bottle of soothing peppermint lotion to invigorate your feet and your spirit... And our special sandal adapters, so you'll never be without your Walkfits. It inhibits and kills fungus and bacteria, so no more stinky, sticky feet. And don't forget, we have holes in the Walkfit to keep your feet cool all the time.

What Are Heel Fissures And How Can I Treat Them?
Last night I was sat grating the hard skin off my feet (as you do!) and my bf was mocking me, and totally grossed out by it. Make sure you pamper your feet properly and provide a good care in order to get smooth and healthy feet. Dry, cracked feet are unsightly and painful.

Nevertheless, some KP victims have keratosis pilaris around the chest, reduce and higher arms, back, thighs, buttocks, calves, and experience, generally, anyplace the place hair can develop. You may want pop the bumps in your pores and skin and have the ability to take away the keratin; nonetheless, it is not going to inflict excellent and can just disappear completely a scar in regards to the popped region so it's not necessarily suggested which you do that. If you take into account the skin situation like a problem, you could have to bear in mind on the proven fact that keratosis pilaris within the chest and also on all components in the body don't have any one cure or therapy. Treating KP is for the aesthetic seem of the pores and skin for most KP sufferers. You will find now strategies and guidelines made to help KP sufferers recover from their stress making their influenced skin look even slightly clearer. Our skin is subjected to much more sun harm as we age. I finally have soft feet.
It may be so severe that people who have the condition are usually kept awake at night because of the pain. Because the calcaneus or the heel bone is the largest bone that can be found in the foot, it usually hits the ground first when the individual walk, causing foot pain. Another cause is due to strain on the ligament at the foot bottom, called plantar fascistic. Athletes also tend to develop heel pain from stress fractures.
Hands at times also get infected with calluses, but the use of pumice stone is not advised for removal of calluses on hands. The process is a bit slow, but the treatment is permanent and guaranteed without any side effect. There are surgical treatments as well where your doctor will cut the hard skin but only few people resort to this option. As far as medication is concerned salicylic acid ointments is often used to remove the hard portions of the skin. Complications caused by calluses should be consulted with podiatrist as it can also cause infection in certain number of ways. The treatment of callus depends upon its nature and severity. But some of the treatments out there are very hard and damaging to your skin.
The important question is how to choose the best one out of so many creams for getting rid of dry skin. I suffer from awful hard skin it will never go away ever I keep it at bay best I can but once a week I have to attack my feet with various devices I own. Scholl Cracked Heel Repair Cream - You still have to file the skin down first but once you've done that its ok but nothing special. Clean your feet using cotton wool dipped in surgical spirit at night. This helps to keep the skin dry and remove cracks. Particular fabrics that socks are made of can cause the feet to sweat more. You have put on your boots because the winter has showed its teeth and then you realized that you have neglected your feet a lot. Exfoliate your feet every week.
Cracked Heels Diagnosis And Treatment
See how much softer and smoother my skin looks in the second photo? Corns and calluses can be painful and frustrating problems in the foot. The stretching foot rocker is a helpful tool in relieving pain associated with lower leg conditions. Alton Beauty has now added Callus Peel to the range of pedicure treatments. Everybody, from school children on can recognize a wart.

The boring bits, like the kneecaps, unless you have a fetish for kneecaps, the sometimes unpleasant parts, like the callous on your foot serving as a hat to your bunion, the parts you just wonder about, like your weenus, and yes, the beautiful aspects, perhaps the eyes, the smile, or the hands. My friend Sergio gave it to me, and he told me that he has had it for 7 or 8 years, and its really special to him. Simply apply the Softener Gel to a Foot Patch. After just a few minutes, use the Scraper to peel and scrap away those ugly calluses. Next for the finishing touch use the file to smooth out the skin and apply the Foot Balm to achieve baby soft supple feet! A manicure involves trimming fingernails, removing excess cuticle, and adding nail polish (with color or just a clear top coat). A pedicure is the same thing for your feet. When you get a facial you get more of a spa experience than just a pedicure or manicure.
If you have diabetes or another condition that causes poor circulation to your feet, you're at greater risk of complications. Corns are smaller than calluses and have a hard center surrounded by inflamed skin. Corns usually develop on parts of your feet that don't bear weight, such as the tops and sides of your toes. Corns can be painful when pushed or may cause a dull ache. Calluses usually develop on the soles of the feet, especially under the heels or balls, on the palms, or on the knees. Calluses are rarely painful and vary in size and shape. They can be more than an inch in diameter, making them larger than corns. When shoes are too tight or have very high heels, they compress areas of your foot. Repeat two to three times; switch feet.
The author of the article recommends the patients suffering from any foot disorder to take services of Nagler Foot Center for satisfying results and reasonable charges. A plantar callus is a thickened amount of skin that can develop on the bottom of the foot where your heel bone connects to your toes. The skin forming the callus can be gray or yellowish in appearance, dry, hard, painful and flaky. To treat a plantar callus, a doctor can trim away the thick skin with a scalpel.

Patients with poor vision cutting nails too deep beneath crease line can lead to skin breakage and in patients with poor blood flow to foot can lead to major amputation.Proper nail cutting techniques should be learnt,toe nails should be cut straight,not beneath creaseline. At the center of a corn is often a very dense knot of skin called a core, which is located over the area of greatest friction or pressure. Firm, dry corns that form on the upper surfaces of the toes are called hard corns. Pliable, moist corns that form between the toes are called soft corns.

Height Lengthening Surgery Questions and Answers | Height Lengthening
Height Lengthening Surgery Questions and Answers | Height Lengthening
What is Height Lengthening and Deformity Correction Surgery?
The Height Lengthening procedure utilizes the newest techniques available to allow the lengthening of your legs, thighs, or a combination of both.? The method consists of a minimally invasive technique that creates a surgical cut in your bone and with gradual lengthening, using an external or internal device, the bone is lengthened to the desired height.? As a result, your height will increase several inches.
Deformity correction surgery is used to lengthen and/or straighten deformed bone segments and also to replace missing bone. The procedures may be performed on both children and adults who have leg length discrepancies or deformities due to birth defects, disease, or injury. ? It also covers patients with bony nonunion (non-healing bone), bow legs, knock knees, foot and ankle deformities, and osteomyelitis (bone infection).
What are the different devices that are used in Height Lengthening?
Depending on your body"s anatomy, the lengthening may need to be performed either in your legs or the thighs.? If the lengthening is performed in the legs, either an external device called the Taylor-Spatial Frame (TSF) or the new PRECICE lengthening device is used to gradually distract and slowly grow the new bone.? Once the desired length in the legs has been achieved using the TSF, an internal rod made of titanium is placed and the external TSF is removed.? This will allow much less time in an external device while supporting the new bone during its consolidation (maturation) phase.
If the lengthening is performed in the thighs, one of two techniques may be utilized:
1) Lengthening Over a Nail (LON): This technique utilizes an external device to distract and lengthen the bone, while an internal rod that is in place serves to protect the new bone that develops.
2) Fully implantable self-lengthening rod:? A new device that has recently been developed, the PRECICE lengthening device, serves to lengthen the bone with its patented internal magnetic mechanism without the need for an external fixation device.
How much height am I able to gain?
If only one segment of your limb is lengthened (the leg or thigh), you can potentially gain up to 4 inches in height; however, most people are able to gain 3 inches without much difficulty or complications.? With the combination of lengthening both thighs and legs, you can potentially achieve up to 16 cm in length.? The limiting factor will depend on your body"s anatomy and how much lengthening the soft tissues can tolerate.
How long is the Height Lengthening/ Deformity Correction surgery?
The surgery for each limb takes approximately 2? hours.? This does not include preop and postoperative anesthesia time, which can take an additional 20 to 40 minutes.
What does the surgery entail?
The height lengthening procedure involves initially placing an internal device or external frame on the limb.? Then a surgical cut is made in the? bone through a minimally invasive technique in order to allow lengthening or correction of any deformities in the legs.
What is the recovery time after surgery?
Some surgeries may be performed as an outpatient procedure with a 23-hour stay at the surgery center or at the hospital.? Some patients may require 2-3 days in the hospital depending on their level of pain and mobility after their procedure.? The day after surgery, patients are encouraged to start walking and putting their full weight on their legs with the support of crutches or a walker.? The amount of time to fully recover depends on how much length needs to be achieved or amount of deformity that needs correcting.? The approximate time to return to full activities is 3-5 months.
How long will I wear the external device?
Only until you gain the desired height that was planned preoperatively.? Once the distraction (lengthening) phase is complete, the internal device (titanium rod) will hold and protect the new bone that has formed.
How are the adjustments on the frame performed?
A computerized schedule will be printed out for you that will instruct you to turn each strut at the appropriate time on a daily basis.
What are the potential complications of surgery?
The most common complications are pin tract infections, which are routinely treated with antibiotics; Joint stiffness may also occur, which will require physical therapy to correct.? Other complications may include nerve injury, vessel injury, and compartment syndrome.? Most of these complications are rare and can be treated with physical therapy or additional surgery.
Do I qualify for the Height Lengthening procedure?
There are a number of factors and certain limitations for whom the Height Lengthening procedure can be performed.? The guidelines include:
No bone disease (i.e. Vitamin D deficiency)No bone infectionPatients cannot have body dysmorphic syndrome
The procedure may be performed on children as well. However, in order to qualify, each case must be taken into consideration on an individual basis. A psychologist may need to evaluate you as well before qualifying for the procedure.
How much does the Height Lengthening surgery cost?
Your initial consultation is $600.? This will include the physical exam, xrays, and a discussion of the best treatment option for your surgical technique. ? The surgery may or may not be covered by insurance depending on your body"s anatomy. If your insurance does not cover the surgery, you will need to pay for it in full before the operation can commence.? Cost of the surgery can vary from $40,000 to $75,000 depending on the procedure, which includes the equipment, surgery fees, hospital fees, and post op visits during the lengthening stage.? The entire cost must be paid in advance of the operation. A more accurate cost estimate will be available once you have visited with the surgeon and determined if you qualify for the surgery.
How do I schedule my Height Lengthening surgery?
The first step is to make an appointment to be evaluated by the surgeon. Then you will have a discussion regarding the Height Lengthening procedure.? Someone from our staff will then contact you to schedule the surgery if you have been accepted as a candidate.